Are you worried about the 2019 MIPS Promoting Interoperability category?
The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) replaced the Medicare Sustainable Growth Rate (SGR), which was how CMS previously controlled the cost of Medicare Payments to physicians. MACRA is aimed at strengthening Medicare access, improving physician payments, and encouraging better patient care among other improvements. Under MACRA, CMS is required to implement a Quality Payment Program (QPP), which offers clinicians and practices two separate tracks: (1) the Merit-Based Incentive Payment System (MIPS) track; and, (2) the Advanced Alternative Payment Model (Advanced APM) track. Both tracks can result in penalties for not meeting certain requirements/benchmarks or incentives for meeting and exceeding requirements/benchmarks.
Depending on specialty and other factors, the majority of MIPS eligible clinicians and practices are eligible to report on the Promoting Interoperability (PI) category to help avoid penalty and earn incentives. Whenever possible, a practice should submit multiple categories including Promoting Interoperability to earn the maximum MIPS Composite Performance Score (CPS) or “MIPS score” possible. The good news for 2019 MIPS eligible clinicians and practices is that, they maintained a 90-day reporting window.
A lot has changed about the PI category from 2018 to 2019 but don’t worry. Join me as we discover the twists and turns CMS has in store for this ever-evolving category.
2015 ONC Certified EHR Technology
The 2019 final rule required that all practices reporting on the PI category in 2019 use 2015 ONC Certified EHR Technology (CEHRT). A 2014 ONC CEHRT or a combination of 2014 and 2015 CEHRT will no longer make the cut. The CEHRT is valid as long as it is certified by the end of the 2019 reporting year (December 31, 2019). When submitting for PI for 2019, you have to include the ONC CEHRT ID with your data submission to CMS, otherwise you will score a zero for the category.
Four PI Objectives and Measures
The base, performance, and bonus measures you knew and loved no longer exist. Instead, there are several measures that are required to be reported on for category scoring, unless certain measure exclusion criteria are met. Report the required measure from each of the four objectives or claim their exclusion(s). Each objective contains one or more measure(s) to report on. The total possible score is out of 110 (with two possible bonus measures worth 5 points each). The maximum reportable score is 100.
E-Prescribing Objective (worth 10 – 20 points)
Uses numerator and denominator data for reporting; contains 1 measure, 2 additional bonus measures:
- E-prescribing measure – (worth up to 10 pts)
- Bonus! Query of prescribing Drug Monitoring Program (PDMP) – (worth 5 points)
- Bonus! Verify Opioid Treatment Agreement – (worth 5 points)
Health Information Exchange Objective (worth up to 40 points)
Uses numerator and denominator data for reporting; contains two measures:
- Support Electronic Referral Loops by Sending Health Information (worth up to 20 points)
- Support Electronic Referral Loops by Receiving and Incorporating Health Information (worth up to 20 points)
Provider to Patient Exchange (worth up to 40 points)
Uses numerator and denominator data; contains 1 measure:
- Provide patients electronic access to their health information (worth up to 40 points)
Public Health and Clinical Data Exchange (worth 10 points)
“Yes”/ “No” statements.
This is an interesting objective in that it has 5 measures to pick from and you must choose at least two. The five measures to select from are:
- Immunization Registry Reporting
- Electronic Case Reporting
- Public Health Registry Reporting
- Clinical Data Registry Reporting
- Syndromic Surveillance Reporting
Measure Scoring
Below is a sample of the new PI scoring system without any measure exclusions:
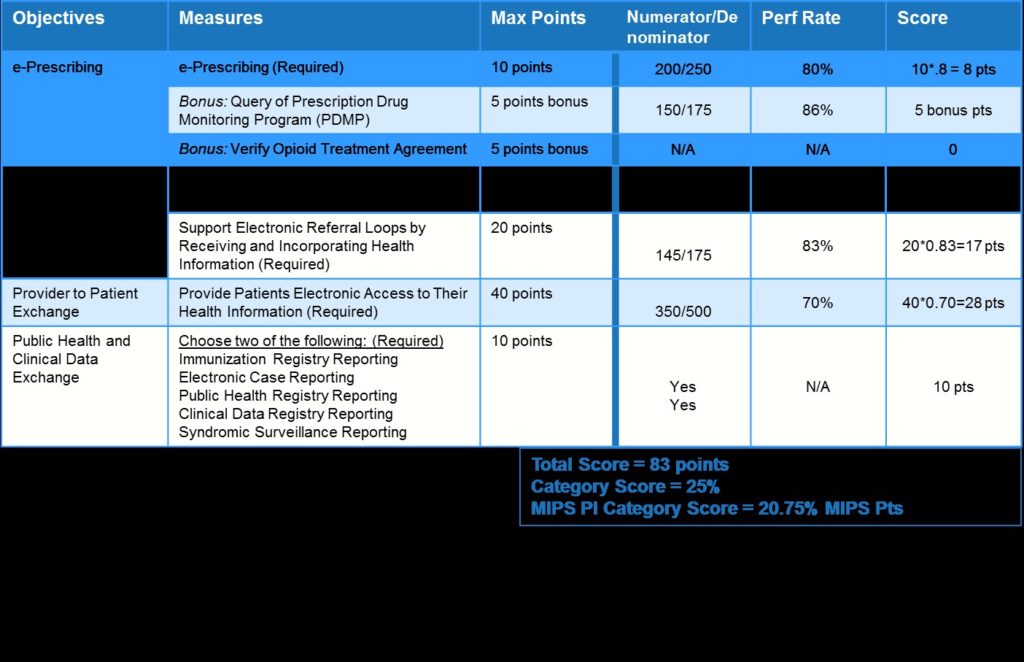
Scoring options are rife for exclusions. Each measure has the option of an exclusion EXCEPT for the Provider to Patient Exchange measure because CMS is really making it a priority for patients to be able to access their health information electronically. If you meet the exclusion criteria for any of the other measures, the points will be redistributed either within the objective or even across objectives.
Reweighting Options
 In some cases, PI can be reweighted (lucky you!) There are 2 ways that the PI category points can be reweighted to the quality category: (1) through an application process; (2) through an automatic designation.
In some cases, PI can be reweighted (lucky you!) There are 2 ways that the PI category points can be reweighted to the quality category: (1) through an application process; (2) through an automatic designation.
Hardship Exception (application-based) Reweighting
If a hardship application is submitted on or before December 31, 2019, the 25 possible PI points will go into the Quality category making it worth 70% of your overall MIPS score.
Automatic Reweighting
Occurs if you’re one of the following types of MIPS eligible clinicians:
- Ambulatory-Surgical Center (ASC)-based MIPS eligible clinician
- Hospital-based MIPS eligible clinician
- Non-patient facing clinicians
- Any of the following clinician types, including: Physician Assistant (PA), Nurse Practitioner (NP), Clinical Nurse Specialist (CNS), Certified Registered Nurse Anesthetist (CRNA)
- Any of the 2019 newly added MIPS eligible specialties, including: Physical Therapists (PT), Occupational Therapist (OT), Qualified Speech-language Pathologist, Qualified Audiologist, Clinical Psychologist, Registered Dietitian or nutritional professional
Additional Requirements
In additional to the 2015 ONC CEHRT and minimum continuous 90-day reporting window, there are attestation statements that MIPS reporters must sign off on with a “yes” in order to get scored under the PI category:
There were a lot of surprise changes to the Promoting Interoperability category in 2019, that were outside of the expected change requiring 2015 ONC CEHRT to get scored on the category. The key is not to get bogged down with the many CMS programmatic twists and turns, when there are experts here to help you understand and report successfully.
The criteria which determine MIPS eligibility are multi-faceted and complex. ReportingMD understands these criteria’s and works with client organizations to optimize incentive performance in the MIPS (and other value-based care programs.)
With the proven experience of our client services team and Total Outcomes Management (TOM™) a powerful measure calculation engine, ReportingMD can help you navigate the complexities of the MIPS program.
We were invited by CMS to help develop the MIPS program, which provides our team with unique expertise and a depth of experience that’s unmatched.
Using TOM™, practices can gain operational visibility to the quality performance of their physicians and avoid CMS penalties for non-compliance. TOM™ aggregates data from multiple sources to identify and manage patient care gaps.
Learn why mid to large sized healthcare organizations turn to ReportingMD for powerful tools that help improve patient care, improve quality outcomes, and maximize reimbursements.

